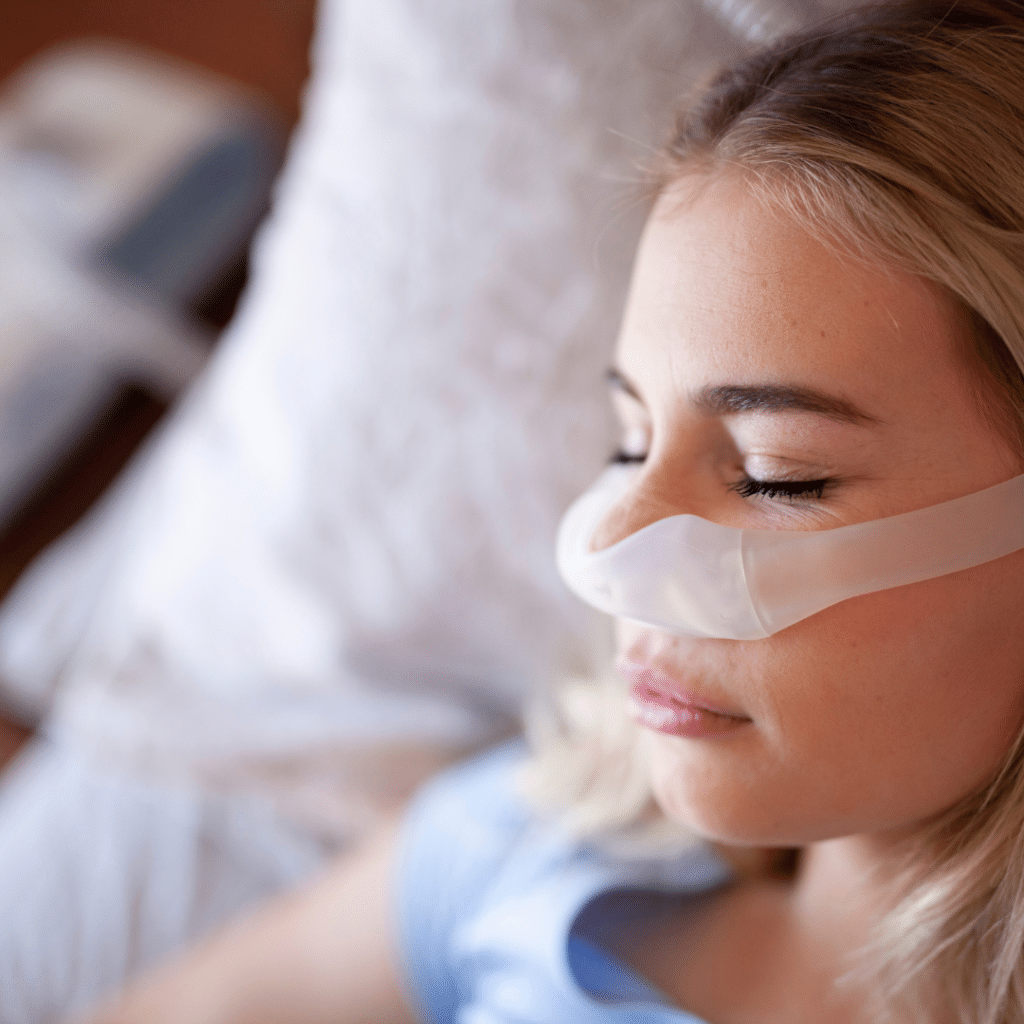
Sleep is a fundamental physiological process that is crucial in maintaining overall health and well-being. The quality of sleep has a significant impact on various bodily functions, cognitive processes, and emotional stability. Sleep disorders are known to disrupt this delicate balance, and sleep apnea stands out as one of the most prevalent and concerning disorders.
Poor sleep increases the risk of cardiovascular disease, weight gain, dementia, type II diabetes, and many other medical conditions. Sleep deprivation can worsen any mental disorder, including anxiety, depression, and bipolar disorder.
Sleep apnea is characterized by repeated interruptions in breathing during sleep, leading to fragmented sleep patterns and potential health complications. While the primary cause of sleep apnea is often attributed to anatomical factors such as airway obstruction, there is a growing body of research suggesting that stress might also contribute to the development and exacerbation of sleep apnea.
This post delves into the complex relationship between stress and sleep apnea, exploring the potential mechanisms underlying their connection and the implications for clinical management.
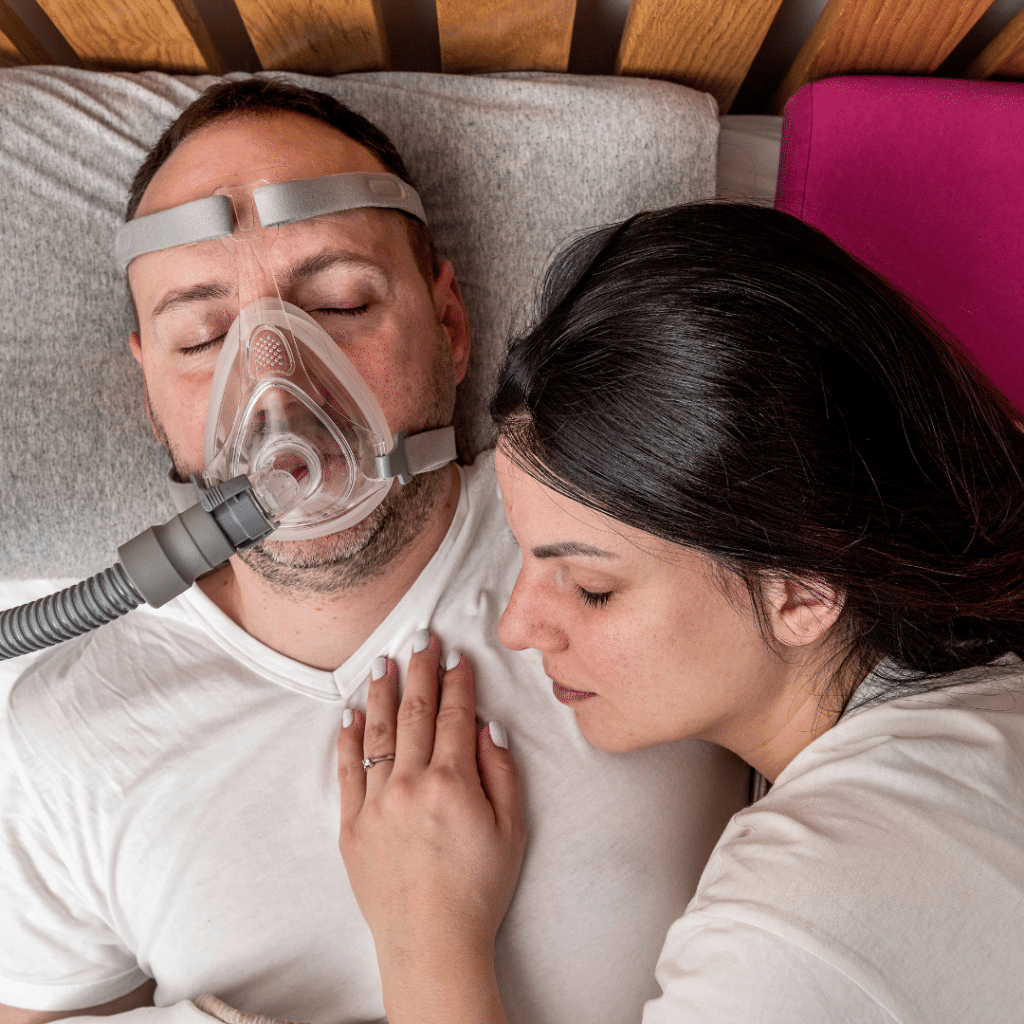
Stress and Sleep Apnea: A Two-Way Interaction
The Physiology of Stress:
Stress is a universal human experience, a natural response to various challenges and demands in life. Whether facing a looming deadline, a public speaking engagement, or a sudden danger, the body’s stress response is a complex cascade of physiological reactions that prepare us to deal with the situation.
The Stress Response Pathway:
The hypothalamic-pituitary-adrenal (HPA) axis is at the stress response’s heart. This intricate system involves coordinating the hypothalamus, pituitary gland, and adrenal glands to release stress hormones. When confronted with a stressor, the hypothalamus signals the pituitary gland to release adrenocorticotropic hormone (ACTH), which stimulates the adrenal glands to produce cortisol, often called the “stress hormone.”
Immediate Physiological Changes:
In the face of stress, the body initiates a fight-or-flight response, preparing to confront the stressor or flee from it. This leads to a series of rapid physiological changes:
- Increased Heart Rate and Blood Pressure: The sympathetic nervous system is activated, causing the heart rate and blood pressure to rise. This prepares the body to deliver oxygen and nutrients to muscles and organs to respond to the impending challenge.
- Dilated Airways: The airways in the lungs widen, allowing for increased oxygen intake. This supports the body’s heightened demand for oxygen during stress.
- Redirected Blood Flow: Blood flow is redirected from non-essential functions, such as digestion, to essential functions like the brain and muscles. This enhances physical and cognitive capabilities.
- Release of Glucose: The liver releases stored glucose into the bloodstream, providing a quick source of energy to fuel the body’s response.
- Heightened Sensory Perception: The senses become more acute, enabling the individual to detect potential threats more effectively.

Long-Term Effects and Chronic Stress:
While the stress response is essential for survival, chronic stress can harm overall health. Prolonged activation of the stress response can lead to a range of health issues, including:
- Cardiovascular Impact: Elevated heart rate and blood pressure over time can increase the risk of heart disease, hypertension, and stroke.
- Suppressed Immune System: Chronic stress can suppress the immune system’s functioning, making the body more susceptible to infections and illnesses.
- Mental Health Concerns: Persistent stress is linked to the development of mental health disorders such as anxiety and depression.
- Digestive Disorders: The diversion of blood flow away from the digestive system can lead to gastrointestinal problems, including irritable bowel syndrome.
- Cognitive Impairment: Prolonged exposure to stress hormones can affect memory, concentration, and cognitive function.

Sleep Apnea: An Overview:
Sleep apnea is a common and potentially serious sleep disorder characterized by recurring pauses in breathing or shallow breaths during sleep. These breathing interruptions can last for a few seconds to minutes and may occur multiple times during the night. As a result, sleep apnea disrupts the normal sleep cycle, leading to poor sleep quality and a range of potential health complications.
Types of Sleep Apnea:
- Obstructive Sleep Apnea (OSA): This is the most prevalent form of sleep apnea. It occurs when the muscles at the back of the throat relax excessively, leading to the temporary collapse of the upper airway. As a result, airflow is obstructed, and breathing temporarily stops until the brain signals the body to awaken slightly and resume breathing. Individuals with OSA often experience loud snoring, gasping, or choking sounds during sleep.
- Central Sleep Apnea (CSA): This type is less common and is primarily characterized by the brain’s failure to transmit proper signals to the muscles responsible for breathing. Unlike OSA, CSA is not usually associated with physical airway obstruction. It often results in abrupt awakenings, shortness of breath, or difficulty staying asleep.
- Complex Sleep Apnea Syndrome (Mixed or Treatment-Emergent Sleep Apnea): Treatment-emergent central sleep apnea occurs when an individual initially has OSA but develops central sleep apnea after receiving treatment with continuous positive airway pressure (CPAP) therapy.
Common Symptoms of Sleep Apnea:
Sleep apnea symptoms can vary in severity and may include:
- Loud Snoring: Especially common in OSA, loud and chronic snoring can disrupt sleep for both the individual and their partner.
- Pauses in Breathing: Witnessed by a bed partner or recorded during sleep studies, these breathing interruptions are a hallmark of sleep apnea.
- Excessive Daytime Sleepiness: Due to fragmented sleep, individuals with sleep apnea often feel excessively tired during the day, leading to difficulties concentrating, staying awake, and performing daily tasks.
- Morning Headaches: Recurring headaches upon waking may result from the decreased oxygen levels associated with sleep apnea.
- Irritability and Mood Changes: Sleep disruptions can affect mood, leading to increased irritability, mood swings, and even depression.
- Insomnia or Restless Sleep: Individuals may have trouble falling asleep or experience restless tossing and turning during the night.
- Awakening with a Choking Sensation: A sudden awakening accompanied by choking or gasping for air can indicate sleep apnea.

The Stress-Sleep Apnea Connection:
- Bi-directional Relationship: Research suggests that the relationship between stress and sleep apnea is complex and bi-directional. Chronic stress can potentially contribute to the development and exacerbation of sleep apnea. On the other hand, the fragmented and poor-quality sleep caused by sleep apnea can also exacerbate stress levels, creating a vicious cycle.
- Impact on Airway Function: Stress-induced changes in muscle tone and respiratory control mechanisms can influence the risk of sleep apnea. Chronic stress may lead to increased muscle tension, including those responsible for airway stability, potentially narrowing the airway and increasing the likelihood of breathing interruptions.
- Neuroendocrine Pathways:The release of stress hormones, particularly cortisol, has been linked to alterations in the neural control of breathing. Cortisol affects the respiratory centers in the brainstem, potentially disrupting the normal regulation of breathing patterns during sleep.
- Inflammation and Immune Response: Chronic stress can contribute to chronic low-grade inflammation in the body. Inflammation is believed to play a role in the pathophysiology of sleep apnea by promoting airway inflammation and compromising the integrity of the upper airway muscles, thereby increasing the risk of airway collapse.

Clinical Implications and Management Strategies:
- Screening and Assessment: Given the potential interplay between stress and sleep apnea, healthcare professionals should consider both factors when evaluating patients. Comprehensive assessments should consider anatomical factors, the patient’s stress levels, and psychological well-being. Different treatment options should be considered, and a sleep specialist may be consulted in severe cases.
- Stress Management: Incorporating stress management techniques into treating sleep apnea could be beneficial. Techniques such as cognitive-behavioral therapy, mindfulness, and relaxation exercises may help reduce stress levels and improve sleep quality. Patients should be questioned about symptoms of anxiety, panic disorder, and other psychological symptoms.
- Collaborative Approach: A holistic approach that involves collaboration between sleep specialists, psychologists, and other healthcare professionals can provide a more comprehensive treatment strategy for individuals with sleep apnea and elevated stress levels. Weight loss strategies and lifestyle changes, including substance abuse treatment, should be explored.

The intricate relationship between stress and sleep apnea underscores the need for a multidimensional approach to understanding and managing these conditions. While sleep apnea’s primary cause is often attributed to anatomical factors, it is becoming increasingly evident that chronic stress can also contribute to its development and exacerbation. The bi-directional nature of this relationship highlights the importance of addressing both anxiety and sleep apnea in clinical practice. Untreated sleep apnea can lead to multiple health issues. Those who think they may suffer from sleep apnea should consult their healthcare provider. Future research is warranted to elucidate the underlying mechanisms further and develop more effective integrated interventions that consider the complex interplay between stress and sleep apnea. Ultimately, a comprehensive approach that recognizes the synergistic impact of stress and sleep apnea on health outcomes can lead to improved patient care and overall well-being.

Michael J. Brown, RPh, BCPS, BCPP
Mr. Brown is a Clinical Pharmacist specializing in pharmacotherapy and psychiatry.
Feel free to send Michael a message using this link.
Disclosure: This post may contain affiliate links, meaning, at no additional cost to you, I may earn a commission if you click on, or make a purchase through a third-party link.

